
Chronic exertional compartment syndrome is one of the most common causes of pain, numbness, and foot drop, most often seen in runners.
Platelet Rich Plasma (PRP) is one of several novel therapies in the expanding frontier of regenerative medicine. Platelets are a critical component of the wound healing process. By isolating growth-factor rich platelets from your blood and injecting them into areas of joint and soft tissue damage, PRP has shown promise in its ability to treat degenerative joint disease and aid in the recovery of soft tissue injuries to tendons, muscles and ligaments.
Platelets play an important role in directing and accelerating your body’s normal healing process, by setting off a chain of events governed by signaling proteins. Platelet proteins, which contain huge reservoirs of growth factors, are key participants in this cascade of healing. These platelet-derived growth factors contribute to the processes of tissue repair and regeneration at the injury site.
There has been a growing body of basic science and clinical research demonstrating the effectiveness of PRP. Reported benefits have included reduced bleeding, diminished pain levels, decreased infection rates, enhanced wound closure, accelerated tissue regeneration, and reduction of overall healing times.
Benefits have been described in a variety of musculoskeletal conditions including chronic patellar, Achilles, elbow tendon injuries, rotator cuff injuries, cartilage lesions in the knee, and osteoarthritis of the knee.
It is important to consult with your physician or healthcare practitioner prior to your procedure for specific instructions. You should be rested and well-hydrated. In most cases it will not be necessary to have someone accompany you on the day of treatment and you should be able to return to work.
You will be requested to discontinue taking blood thinners, anti-inflammatory medications such as ibuprofen and naproxen, as well as aspirin, up to 5 days prior to the procedure and for at least 1-2 weeks following. These medications will counteract the effects of PRP.
A PRP injection is usually performed on an outpatient basis. A small amount of blood is drawn and then placed into a centrifuge. The centrifuge spins and concentrates the platelets in roughly 15 minutes. With this technique, it is possible to achieve platelet concentrations up to eight times higher than normal, which can then be used for the procedure.
Your physician will use an antiseptic to clean the site of the injection. Your skin and muscle tissue will then be numbed with local anesthetic. Image guidance, with either dynamic ultrasound or fluoroscopy, may be used to visualize the injured area and assist in precisely placing the injected material into the desired location. It is common to experience mild discomfort during this part of the procedure. The entire process usually takes about one hour.
Following the injection, and after the anesthetic wears off , you may experience worsening of pain for several days, as the introduction of PRP will stimulate an inflammatory reaction at the site of the injection. This is a desired effect and it is important to avoid ice and anti-inflammatory medication for up to one week. Your physician may recommend acetaminophen or analgesics to manage your discomfort. Adverse effects are uncommon with this procedure. Because PRP is composed of your own blood, there is a minimal risk of disease transmission and allergic reactions.
Post-injection rehabilitation will depend on the nature and extent of the injury. Your physician may suggest that you use a walking boot, knee brace and/or crutches for the lower extremity or a sling for the upper extremity to immobilize the treated area. Stretching, light resistance exercises and physical therapy may also be prescribed. It is important to consult with your physician prior to resuming normal activity or exercise.
PRP injections are often repeated. While symptoms may improve after a single injection, it is not uncommon for patients to receive a series of up to three to five injections over several months to maximize the benefit of therapy.
301.493.8884
Dr. Mark D. Klaiman, MD
Monday – Friday 8am – 5pm
301.244.9099
Dr. Haim S. Hechtman, DPT
Monday – Thursday 7am – 7pm
Friday 7am – 5pm,
Saturday 8am – 1pm
“When I learned that my two favorite practitioners—who gave me back a normal, pain-free life—were joining their practices I thought, what a winner…..”
– Jane Stanley



Chronic exertional compartment syndrome is one of the most common causes of pain, numbness, and foot drop, most often seen in runners.
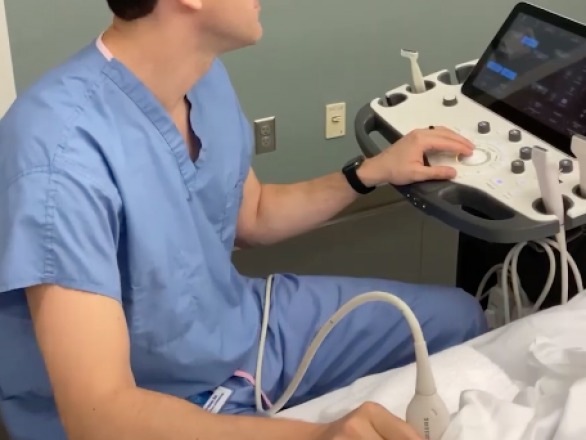
Hip arthritis is one of the most common causes of groin pain in patients. To diagnose it, we can use ultrasound. Ultrasound
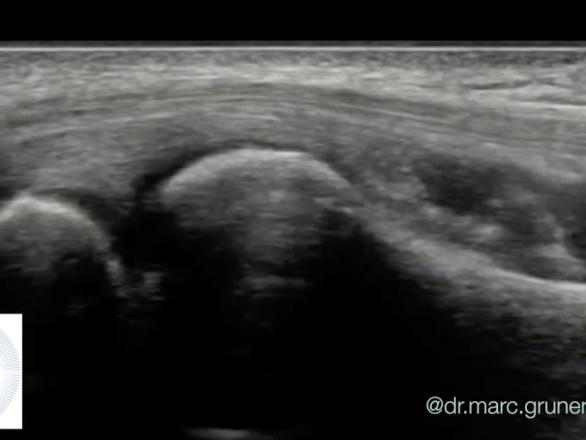
Tennis elbow is one of the most common causes of elbow pain. The condition is also sometimes referred to as lateral epicondylitis.
Starting and sticking with a rehabilitation regimen has its challenges during the pandemic. Here are some ways to continue to progress.
|
We are pleased to offer digital patient referrals.
|