
Chronic exertional compartment syndrome is one of the most common causes of pain, numbness, and foot drop, most often seen in runners.
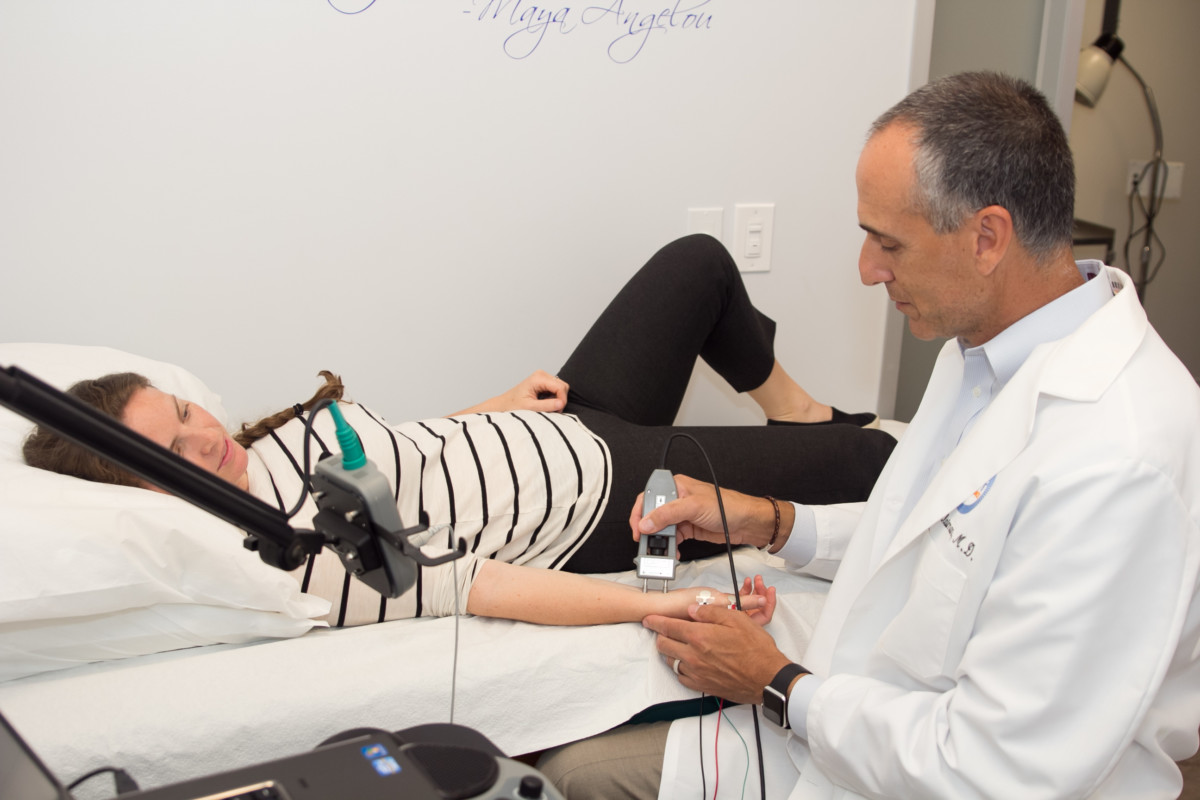
Electrodiagnostic medicine is the study of nerve and muscle diseases. To determine whether your nerves and muscles are working properly, your doctor may refer you for this specialized nerve testing, generally performed by physicians in neurology and physical medicine and rehabilitation. The examination typically includes a Nerve Conduction Study (NCS) and a Needle Electromyography (EMG) test. The results of the electrical examination will help your doctor diagnose your condition and determine the best course of treatment.
If you experience the following symptoms or conditions, you may be referred for electrodiagnostic testing:
• Numbness/Tingling
• Muscle Weakness
• Neuropathy
• Carpal Tunnel Syndrome
• Neck or Low Back Pain
• Sciatica
• Radiculopathy
• Stenosis
Nerves work like electrical cords. They send signals to your brain from your body and from your brain to your muscles. Your muscles are the tissues in your body that make you move.
When functioning properly, the nerves send electrical impulses to the muscles. A nerve disorder means that signals are not getting through like they should. A muscle disorder means that muscles aren’t responding to the signals correctly.
During the NCS, your physician applies small electrical stimulations close to your nerve(s) to study how the nerve works. These impulses cause a quick, mild, tingling feeling. Any discomfort is temporary and the stimulus is not strong enough to cause any damage to your body. Your physician may test several nerves during the course of the study.
During the EMG test, a thin, sterile needle is inserted into several muscles. Your physician is then able to hear and see how your muscles and nerves are working by the way electrical signals travel from the needle to the EMG machine. The only muscles tested are those needed to help determine the nature of your problem. A new needle is used for each patient and is discarded after the examination. There may be a small amount of pain with each needle insertion, however you will likely not experience any residual discomfort after the procedure.
You are being sent for this evaluation because you likely have numbness, tingling, pain, weakness, or muscle cramping in one or more extremities. Your physician will use this examination to determine if your muscles and/or nerves are damaged and, if so, how to treat you.
Tell your physician performing the tests if you: take aspirin or blood thinners (like Coumadin), have a pacemaker, or have hemophilia. On the day of the test, take a bath or shower to remove oil from your skin and do not use body lotion.
Each study is designed especially for you based on your symptoms. The length of the test is different for every patient. The examination usually takes 30-60 min. You may perform normal activities like eating, driving, and exercising before and after the tests. There are no lasting side effects.
Both components of exam can cause momentary discomfort. This varies significantly based on the skill of the physician administering the tests and on the patient’s individual tolerance. We take exceptional care to make the experience an acceptable one and the majority of our patients have little difficulty.
After the tests are complete, your physician will analyze the results and send a report to the referring physician within 24-48 hours. Preliminary results may be conveyed to you at the time of the studies. You should communicate with the physician that recommended the testing to discuss the final interpretation and to determine the next steps in your care.
301.493.8884
Dr. Mark D. Klaiman, MD
Monday – Friday 8am – 5pm
301.244.9099
Dr. Haim S. Hechtman, DPT
Monday – Thursday 7am – 7pm
Friday 7am – 5pm,
Saturday 8am – 1pm
“When I learned that my two favorite practitioners—who gave me back a normal, pain-free life—were joining their practices I thought, what a winner…..”
– Jane Stanley



Chronic exertional compartment syndrome is one of the most common causes of pain, numbness, and foot drop, most often seen in runners.
Hip arthritis is one of the most common causes of groin pain in patients. To diagnose it, we can use ultrasound. Ultrasound
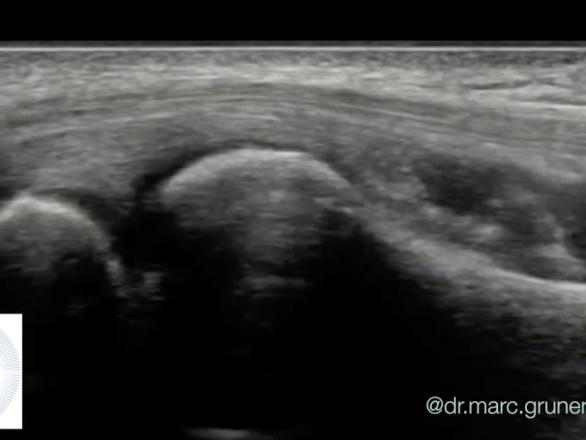
Tennis elbow is one of the most common causes of elbow pain. The condition is also sometimes referred to as lateral epicondylitis.
Starting and sticking with a rehabilitation regimen has its challenges during the pandemic. Here are some ways to continue to progress.
|
We are pleased to offer digital patient referrals.
|