Managing TMD/ TMJ (Temporomandibular Joint Disorders)
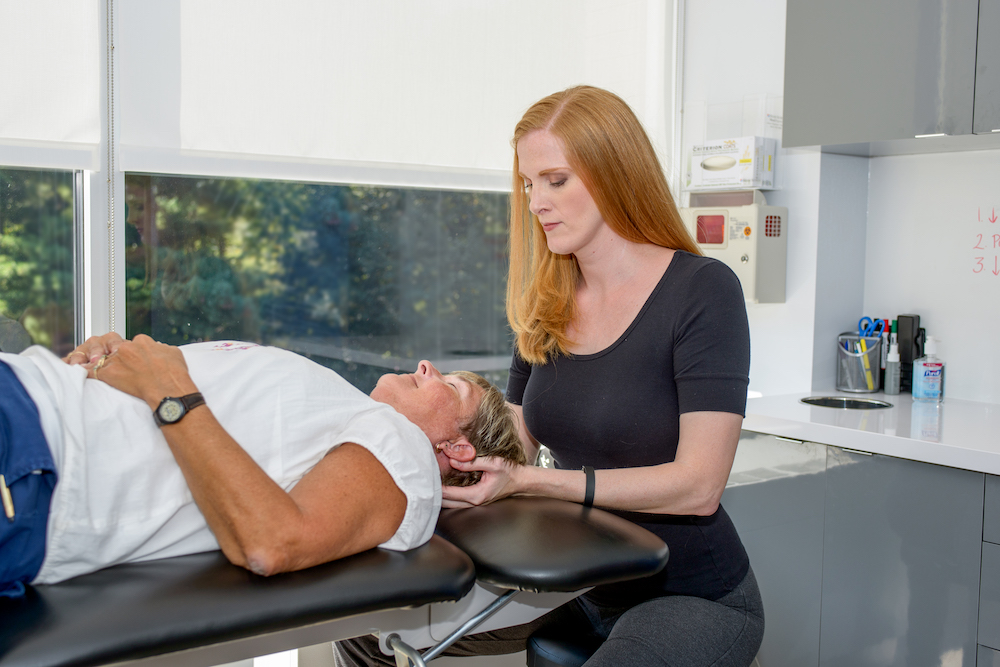
Point Performance’s Dr. Sara Squires Davis works on a patient suffering from TMJ/ TMD.
When you’re stressed, as many people in the Washington, D.C. are, you may find your teeth clenched and eventually a lot of pain harboring in the back of your mouth. Chances are you suffer from Temporomandibular Joint Disorder, named for the hinge in your mouth (the temporomandibular joint) that connects your jaw to your skull and allows your mouth to open and close.
TMD, sometimes called TMJ for the joint, is either caused by injury (whiplash or heavy blow to the face), arthritis, or constant clenching of the teeth from stress. Pain is felt in the back of the face, where the jaw connects, and in the teeth. The face may be swollen, and cause headaches. Sometimes it’s mistaken for root canal by the dentist because the pain is so severe.
If dental practitioners haven’t cut the nerve yet, they may have offered a nightguard to prevent further damage to the teeth that occurs from unconscious grinding during nighttime sleep. Sometimes, however, additional therapy is needed to help an individual manage stress and loosen the jaw during the daytime.
Treating the mouth is difficult because it opens and closes about 20,000 times a day, mostly just for talking and eating. It doesn’t have a real chance to rest, except at night when you’re sleeping. If you’re grinding your teeth, however, your mouth won’t have a moment’s rest then, either.
When patients come in for TMD, the physical therapist will ask about lifestyle habits, job stress, family issues, and whether they have a way to manage their stress through exercise or wellness. The therapist will tailor the treatment depending on the reason behind the TMD, whether it’s for general stress or for a car accident, for example.
The therapist will study the individual’s past medical history, measure the mouth opening and the bite and examine how the teeth touch each other. She’ll look at the tongue and inside of the cheeks, which can tell a lot about whether the person bites his or her cheeks or suck them in as a compensatory strategy for stress. She’ll also analyze the spine to rule out any chance that the pain is actually from the neck or shoulder rather than originating from the TMJ. The therapist works to relieve pain from the soft tissue in the jaw and the neck. Sometimes she’ll apply dry needling to provide immediate relief and a noticeable difference in the bite.
During treatment, patients have to avoid chewy foods, such as bagels, nuts, and gum. It’s also a good time to cut nail-biting as a habit too.
Most treatment is manual therapy combined with exercises to do at home. For those with asymmetrical jaw openings, one exercise involves practicing holding a pen in the mirror and opening and closing their mouths, slowly and symmetrically, to help take the strain off the jaw.
After a period of regular treatment of about four to six weeks in duration, TMD patients will notice a real change in their pain—it’s gone!—and their stress levels improved dramatically, even if the rest of their job and home life remain the same. Patients come in weekly and then may choose to return regardless of the pain for regular maintenance and prevention.
If you suffer from TMD, don’t wait for the pain to disappear, because likely it won’t. Instead, schedule a visit with a TMD-focused physical therapist or dentist, who may refer you to a physical therapist as well.
